First, a brief but necessary introduction:
Negative patient reviews are a fact of life. You can’t avoid them, and you shouldn’t ignore them. Instead, deal with them by leveraging the techniques you’ve honed as a physician – diagnose the problem, synthesize a cure, and administer treatment. At Medical Justice, we’ve helped our clients respond to thousands of negative patient reviews. Today, we are sharing the essentials ingredients with the public – addressing reviews from anonymous patients slamming doctors online.
If you are preparing a response to a negative patient review, schedule a consultation with our Founder and CEO, Jeff Segal, MD, JD. We offer consultations specific to patient reviews. We’ll help you defend your practice’s reputation and keep you from stepping on one of the dozens of regulatory landmines that catch doctors and practice managers off-guard. Use the form below to schedule your consultation.
Our hope is that physicians will exit this page having learned how to respond to negative patient reviews in a way that is effective, concise, respectful of their limited time, and HIPAA compliant. We’ll achieve this end by providing readers with several guidelines and real-life examples. Additional resources are available for download within the article.
Now that you know the agenda – let’s start by reviewing the essentials…
How to Respond to Negative Patient Reviews: The 5 Golden Rules to Follow
Responding to negative patient reviews is a time-consuming process. There are also regulatory landmines doctors must avoid. Some are obvious: Never reveal information about a patient’s treatment without their written authorization. Never identify the author of a review as your patient. Never post billing information online. Others are not as obvious.
When writing a response to a negative patient review, you must remember…
1. A model response shows the practice is reasonable and isn’t in a debate.
2. A model response educates the public.
3. A model response addresses the concerns raised in the review.
4. A model response takes the conversation offline.
5. A model response does not address the author directly.
Write these rules on a piece of paper and share them with your staff. The employee responsible for finding and responding to negative patient reviews should commit these to memory.
The next part of this lesson involves carefully dissecting several real-life examples; examples of negative reviews and examples of model responses. Consider how the examples incorporate all five of the principles outlined above. We’ve prepared a total of four examples, organized into sets of two.
The first set teaches physicians how to respond to negative reviews that result from medical complications. The second set provides instruction on how to respond to negative reviews that result from unexpected costs.
Disclaimer: All examples featured in this piece were collected and posted online by our online reputation management platform, eMerit. The model responses were written by our account managers in collaboration with our clients. We should mention most of the feedback our clients collect is positive. However, we have never filtered reviews. We believe the practice of filtering patient reviews is deceptive. Professional licensing boards regulate advertising and marketing. To such boards, filtering reviews can be perceived as false and deceptive advertising. Further, Google follows this guiding principle in its new E.A.T rules. If you are unfamiliar with E.A.T., we suggest reading this article published by SterlingSky. The penalties can be harsh. You’ve been warned.
That said – let’s dive in…
So – How Do You Respond to a Negative Patient Review that Resulted from a Medical Complication?
Most medical/surgical procedures are completed without issue. The patient is satisfied with the results and renders payment in a timely fashion. The patient moves on, and so does the doctor. Other times the patient exits the practice feeling dissatisfied either because of objective or subjective concerns. An objective concern is a complication, expected or unexpected. A subjective concern is a mismanaged expectation. This may spark exchanges like the example depicted below…

Most medical/surgical procedures are completed without issue. The patient is satisfied with the results and renders payment in a timely fashion. The patient moves on, and so does the doctor. Other times the patient exits the practice feeling dissatisfied either because of objective or subjective concerns. An objective concern is a complication, expected or unexpected. A subjective concern is a mismanaged expectation. This may spark exchanges like the example depicted below…
“While we are sympathetic toward patients who do not see their desired results, we must emphasize that Dr. [BLANK] is board certified through the American Board of Plastic Surgery for plastic and reconstructive surgery in [BLANK], [BLANK]. We hope that readers understand that unfounded allegations like in the above review serve only to start harmful rumors.”
The practice has taken a defensive stance, but it is not an emotional one. They are simply stating facts. The practice acknowledges the patient’s dissatisfaction without divulging unnecessary information. They are content to keep “their side of the story” to themselves.
At a glance, this sounds like a terrible tactic. There are, after all, two sides to every story. Sharing your side of the story may offer the public insight into the clinical aspects of your care. Your side of the story may vindicate you – if not in the eyes of patients, perhaps in the eyes of your fellow physicians.
The temptation to tell all is strong. Still – don’t do this. You’ll get burned.
Imagine a situation where a patient and a doctor are arguing. For the physician to tell his side of the story, what must he do? He must reveal details about the patient’s care. This is a potential HIPAA violation.
Therefore – a physician should never attempt to tell “his side of the story” when responding to an online review unless the patient has provided the physician with expressed written consent. Unless his audience is clairvoyant, the surgeon can’t share his thoughts without creating a public record of the patient’s care. Irritating? Absolutely. Can you still demonstrate your clinical expertise to the public? Absolutely. But there’s an optimal way to do it. We’ll explain how – let’s return to the above example.
When the patient calls into question the physician’s qualifications, the practice refutes the claim, as we saw above. But then they take an extra step…
“Additionally, his well-honed skills have earned him much recognition, such as being voted one of ‘America’s Top Surgeons’ in 2014 and 2015 by the Consumers Research Council of America.”
Perhaps this is more information than is necessary to refute the patient, but that’s the point. Use negative reviews as an opportunity to highlight your qualifications. The response also provides the public with some general insight into the medical complication that triggered the negative review.
“Breast implants bottoming out, though uncommon, is serious and does happen from time-to-time. It’s hard to determine one reason why bottoming out occurs, but contributing factors can include weak breast tissue, smoking, large amounts of weight loss, or even exercising without a support bra.”
This is how you demonstrate your clinical expertise to the public. Be general, and do not address the author of the negative review. The practice never refers to the review’s author as “you.” In fact, the practice barely refers to the patient at all. This is by design. When drafting your responses, you must remember: The author of the review will read your response. Your goal is to resolve his/her concerns. But the author of the negative review is not the only patient who will read your reply. It may be seen by hundreds of prospective patients. So, it pays to respond to negative reviews in a genial manner.
We’ll close our analysis of this example by examining the practice’s closing remarks:
“Any patient who has experienced their implants bottoming out is encouraged to contact our office so we can discuss a revision surgery.”
The purpose of this closing statement is twofold. For one, it addresses the concerns that inspired the negative review. The patient is unhappy with her results and is seeking a remedy. The remedy the practice offers is a revision surgery. Not a free surgery, or a discounted surgery, but a surgery. Perhaps it will be free. Perhaps it will be discounted. But those are details to be worked out at the practice’s discretion. The point is the patient posted with a problem and presumably left with an answer.
Lastly: the closing statement takes the debate offline. The patient’s instructions are clear. If she wants to schedule a revision, she must contact the office directly. Taking the debate offline puts the practice in control and reduces the likelihood the patient’s personal information will be spilled online. And if the doctor-patient relationship continues to sour, it may be best for all parties if doctor and patient parted ways. Our sibling article explains how this must be done in detail: Perfecting the Patient Dismissal Letter.
Let’s examine another example. Like the first, the exchange below depicts a patient who is not satisfied with their care. We suggest reading the response below and then reviewing the five “golden rules” described in this article’s opening paragraphs. Treat it like a test – see if you can identify how the response employs all five in order to achieve a positive end result.
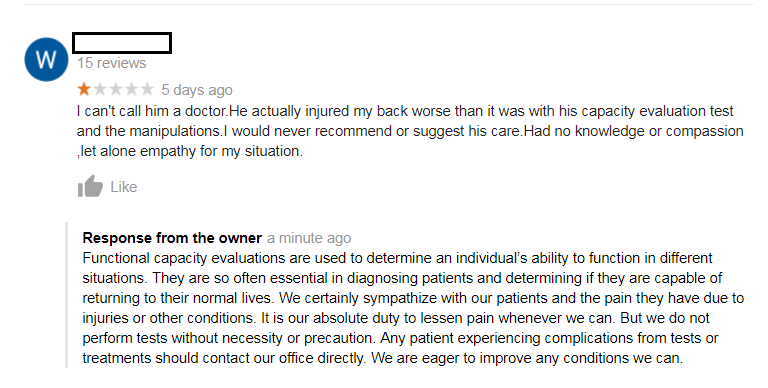
The response paints the practice in a rational light by explaining why treatment described in the negative review (functional capacity evaluations) is necessary. This is done without addressing the author of the review directly. Opening with a clinical truth will keep your emotions out of the response and your focus on educating the public. When you can, share a detail about your practice’s mission statement or payment protocols. In the example above, the practice educates the audience by including the following statement in their response:
“We certainly sympathize with our patients and the pain they have due to injuries or other conditions. It is our absolute duty to lessen pain whenever we can. But we do not perform tests without necessity or precaution.”
The benefits of such a statement are obvious. It sets a certain expectation. And that expectation is, paraphrased, simply this: “We do not perform needless procedures.”
The next priorities are addressing the concerns raised by the review and taking the debate offline. The patient is seeking a solution to their pain. The practice addresses this concern by telling the patient to contact their office directly for assistance.
Next, the cost of treatment is a common point of contention for patients. Let’s shift our focus and discuss the best way to respond to such reviews, starting with the example below…
So – How Do You Respond to a Patient Upset By the Cost of a Procedure?
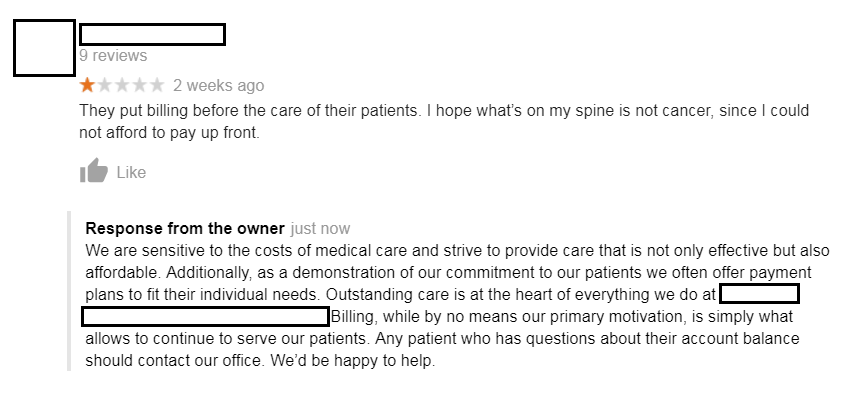
For the sake of brevity, we’ve condensed our analysis into five key points – we trust you are now familiar with them.
How does the response demonstrate to the public the practice is rational?
“We are sensitive to the costs of medical care and strike to provide care that is not only effective but also affordable.”
“Billing, while by no means our primary motivation, is simply what allows us to continue to serve our patients.”
We’ve said it before, and it bears repeating: The best way to sanitize your responses is to deal strictly with facts. Speculative statements are easily misinterpreted by patients and may inspire a string of toxic replies. Both above statements are facts. The first explains the mission statement of the practice. The second acknowledges a universal truth – services cost money to render. A hard point to argue.
How does the response educate the reader?
“Additionally, as a demonstration of our commitment to our patients we often offer payment plans to fit their individual needs.”
In our first example, the practice educated the public by sharing information about a typical surgical complication: breast implants bottoming out. This information was relevant to the patient’s critique and could be shared without revealing specific information about the patient’s care.
In this second example, the source of the complaint is not a medical complication. The patient is complaining about the cost of the procedure. If you receive a complaint like this, educate the public by revealing how you help patients pay for their procedures. In the above example, the practice educates the public by revealing that it allows patients to pay for their care through customized payment plans.
How does the response address the concerns raised in the review?
“Any patient who has questions about their account balance should contact our office. We’d be happy to help.”
How does the response take the conversation offline?
See above. Any invitation to contact the office directly will achieve this end.
Does the response address to the patient directly?
No. Non-specific statements such as “our patients” and “any patient” should be your go-to substitutes for pronouns such as “You”, “She”, and “He.”
Let’s examine one more example. Like the example above, it depicts a patient who is dissatisfied with the cost of their care. There is one big difference, however. The dispute below involves a third-party: the patient’s insurance carrier.
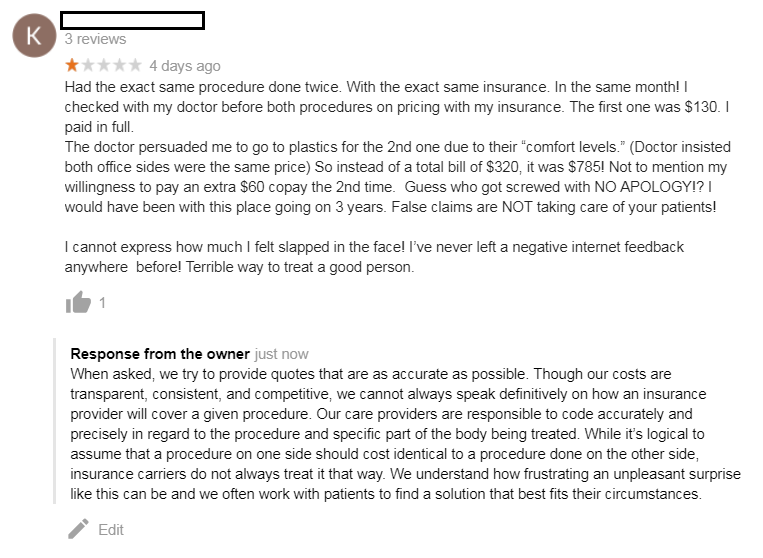
Responding to this kind of negative review can be difficult, as it requires the practice to enter a space where neither the patient nor the physician has complete control. Attempt to manage the online narrative by presenting the patient (and the public) with facts about your practice – write what you know.
“When asked, we try to provide quotes that are as accurate as possible. Though our costs are transparent, consistent, and competitive, we cannot always speak definitively on how an insurance provider will cover a given procedure.
We understand how frustrating an unpleasant surprise like this can be and we often work with patients to find a solution that best fits their circumstances.”
When done thoughtfully, this information can be used to educate the public and position your practice as a business that is patient, rational, and sensitive to the needs of patients. This response also addresses the patient’s concerns and takes the debate offline. If the patient wants to discuss his/her circumstances with the practice, the best way to start that conversation is by getting off the internet and contacting the practice directly. The practice has not promised anything, which is wise, but it is not stonewalling, either. The outcome, favorable or unfavorable, will be determined by the private conversation that takes place between the patient and their care provider.
And with that, we’ve come to the end of our list of examples. While we believe the above four analyses are detailed and insightful, we recognize they are not exhaustive. There are many more reasons why patients write negative reviews. If you are dealing with negative patient reviews, schedule a consultation to learn how we can help you protect your online reputation.
Learn how Medical Justice can protect you from medico-legal mayhem…
Take Advantage of Our Review Monitoring Service
With eMerit, we help you automate review collection and posting to improve your online reputation.
Consult with a Medico-Legal Expert
Medical Justice Founder and CEO, Jeff Segal, MD, JD and our expert team provide consultations to doctors in need of guidance.
Meet the Experts Driving Medical Justice
Our Executive Team walks with our member doctors until their medico-legal obstacles are resolved.





I’ve found that every single practice in our geographical area gets DESTROYED by bitter people- not to mention every business that I personally frequent and love (restaurants, veterinarians, landscapers etc.) so I’ve learned to take reviews with a grain of salt. We’ve been personally threatened and had a gun pulled on us before- for completely unreasonable “justifications.” We are becoming less and less a society of adults and more an entitled and depressed/irritable group of whiners. This just seems to be the status quo for all businesses- the best thing you can do is ignore the ridiculous rants and focus upon the majority of patients who are beyond happy with the care they receive.
Great article Dr. Segal as always and an extremely important topic.
This one hits home to me. About 8 years ago, I had a 31 yo white female, come in my offiice and told me she was on Medicare disability for “fibro” and instertitial cystitis, and as a result urinated so often she could not keep a job. I had to have a red flag in my head as I told her, after she request her 90 “hydros” she gets a month for her “fibro” that I felt she needed MY routine work up and review of previous docs records. She got mad and stormed out of office. One of my nurses noted this patient as they both barrel raced horses often at the same rodeo. I kept thinking poor horse was getting peed on every race. Poor horse.
Here is my point …I subscribe to all services offered by Medical Justice, as well as updates from BS sites like RateMD.com. I think it is important to frequent these sites. It just happened that I checked a site and what do you know, a slam against me by a patient who slammed me for not giving opiates for “fibro” and “what’s next, he doesn’t believe in interstitial cystitis????””
Well I also happened to refer to a rheumatologist for his thoughts on her “fibro” and the week after I saw this patient…. there is a post with ..not to
Repeat the exact story and timeline above.
I happened to see this patient walking towards me in the grocery line, not recognizing me in my hat and Muck boots in the snow, And I said “well hello ‘Michelle’….I saw your post about me on the internet and you should be hearing from my lawyers and IT specialist . Also, my Nurse who rodeos with you, sent a video of you barrel racing to medicate. (All BS), “Happy shopping, might want to use coupons because me and my attorney are t cheap and we don’t play softball!!”
The look on her face, priceless
For everything else, there is Mastetcard! Ha
True story, look Mark Williams Arkansas on RateMD.com at the very first post on me…then oall the positive comments!!
Mark
Unfortunately, Medical Justice was not in existence when I was practicing. I sure could have used this advice then! Internet and reviews are an enormous challenge. It actually takes special “skills” to know how to deal with this.
Their advice is sound. I wish it was around when I needed it.
Michael M. Rosenblatt, DPM
Thank you for providing screenshots and great examples on how we can respond to negative reviews! I definitely agree with the advice to take it offline. Concerns can get resolved much faster either on the phone or in person.
Very nice overview article on sound management of one of today’s social media giants: online reviews. Keep up the good work.